Pfizer's COVID-19 pill reduces risk of being hospitalized or dying by 89%, company says
Pfizer hopes this pill will be available to the public by early next year.

NEW YORK -- A course of pills developed by Pfizer can slash the risk of being hospitalized or dying from COVID-19 by 89% if taken within three days of developing symptoms, according to results released Friday by the pharmaceutical company.
In a study of more than 1,200 COVID-19 patients with a higher risk of developing serious illness, people who took Pfizer's pills were far less likely to end up in the hospital compared to people who got placebo pills.
None of the people who got the real pills died, but 10 people who got placebo pills died, according to results summarized in a Pfizer press release.
Pfizer CEO Albert Bourla said in prepared remarks that the data suggest the pill-based treatment, if authorized, could "eliminate up to nine out of ten hospitalizations."
Infectious disease experts cautioned these results are preliminary -- only described in a press release and not in a peer-reviewed medical journal -- but they represent another promising development in the search for effective and easy-to-administer COVID-19 pills.
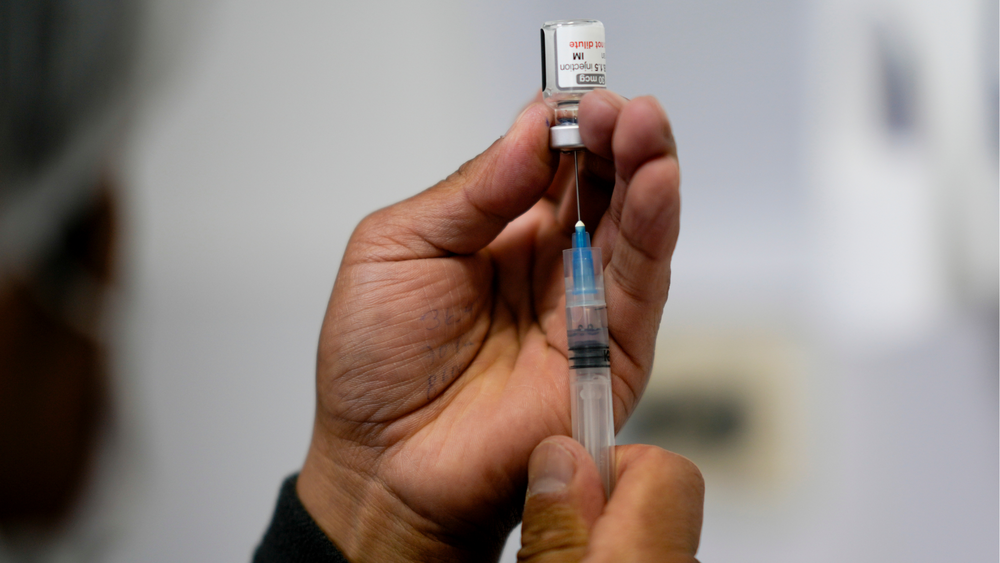
Right now, the only authorized treatments are given via intravenous infusion.
"Having an oral therapy is critically important," said Dr. Carlos Del Rio, the executive associate dean and a global health expert at the Emory School of Medicine.
"If we can get patients to start treatment early before they progress to severe illness and unfortunately death, everyone wins in the fight against COVID," said Dr. Simone Wildes, a board-certified infectious disease physician at South Shore Health and an ABC News contributor.
Infectious disease specialists stressed that these pills are not a replacement for a vaccine -- by far the safest and most effective way to reduce the risk of being hospitalized with COVID-19.
But they may make a big difference if given quickly to people after getting COVID-19, especially the immune compromised, or in places where a vaccine is not available.
Pfizer's pill-based treatment "would be a good drug for patient with COVID and high risk of progression, vaccinated or not," said Del Rio, "although the vaccinated were not included in this study."
Another company -- Merck -- is ahead of Pfizer on developing a COVID pill treatment, having already applied with the Food and Drug Administration for authorization. Emergency use authorization for the Merck treatment may come before the end of the year.

Merck's treatment reduced the risk of hospitalizations and deaths by 50%. This could indicate Pfizer's treatment has an edge on efficacy, but experts cautioned against comparing the studies directly because they were designed in different ways, and measured different so-called "primary endpoints."
"We need to be cautious comparing studies," said Dr. Todd Ellerin, director of infectious diseases at South Shore Health and an ABC News Medical Contributor. But, Ellerin said, it's "great that there is another oral polymerase inhibitor that appears highly effective in symptomatic high-risk outpatients."
The FDA analyzes safety and efficacy before authorizing any medication.
The FDA's advisory committee is set to review Merck's application on Nov. 30. Merck CEO told CNBC at the end of October that the company is ready to distribute 10 million courses of treatment by the end of the year.
Pfizer, meanwhile, plans to start sharing the data with the FDA "as soon as possible."
This Pfizer data is from one of three clinical trials that the company is running. The results from the other two trials are expected by the end of the year. Pfizer then plans to submit all the data and seek authorization at that time, meaning the new medication may be available in early 2022.
Using lessons learned from other infectious diseases, experts said it might one day prove beneficial to combine different antiviral treatments.
"Pfizer oral drug is an investigational SARS-COV-2 protease inhibitor antiviral therapy," Wildes said. "We have used protease inhibitors drugs in our HIV patients and they have worked well."
"Big picture is this is similar to HIV and [hepatitis C] where we have different antivirals," Ellerin added. "There may be an opportunity for combination therapy in the future."